Home/Articles
/ Periodontology /
Reena’s Notes: An Overview on Recession & Infrabony Defects with Dr Roberto Rossi
March 9, 2015
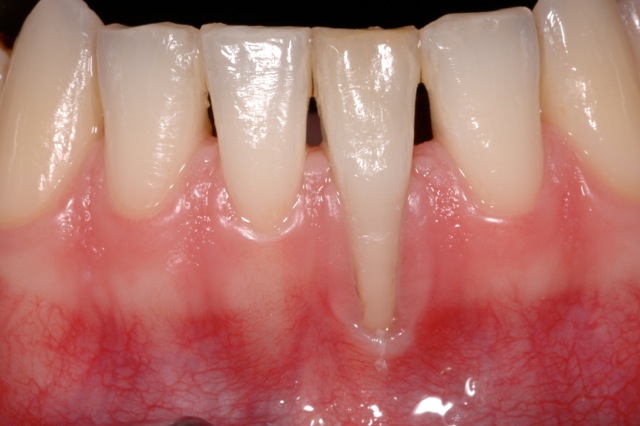
Recession (Soft tissue)
- Aetiology of recession – thin biotype, improper brushing technique, excessive plaque build up, unfavourable anatomy, iatrogenic dentistry.
- Pathogenesis – loss of integrity of epithelium, connective tissue destruction, epithelial migration and reunion of oral and sulcular epithelium.
- Goals of biomimetic periodontal plastic surgery – root coverage, natural colour and texture, maintain position of mucogingival junction.
- There are a number of surgical options for the treatment of recession defects, each with its own advantages and disadvantages.
- Free gingival graft – satisfactory root coverage but often a poor colour/texture match.
- A connective tissue graft is more common and overcomes the problems associated with the free gingival graft.
- Addition of growth factors can be useful if there is a lack of harvesting tissue. A high platelet count is required for this and so this needs to be checked beforehand. The patient’s blood is centrifuged, a super clot is created (blood clot on the root surface) and the flap coronally positioned.
- Derma is a collagenated porcine dermal matrix, which can be used in a similar way to the connective tissue graft (Fischer et al 2014). It may be helpful for more extensive cases of recession when it is difficult to harvest a large area of connective tissue.
- The use of tunnelling allows minimally invasive surgery.
Infrabony (Hard tissue)
- Infrabony defects are classified according to the number of walls.
- 3 walled defects have the optimal anatomy for regeneration, a blood clot or graft is well contained and these cases have the best prognosis.
- 2 walled defects – the missing third wall is usually the buccal plate and a membrane can be helpful here.
- Combination 2 and 3 wall defects – graft the vertical component and use a membrane on the 2 wall component.
- Treatment – autogenous bone, allografts, alloplasts or xenografts.
- Autogenous bone – where possible this is the gold standard. Another site is required to harvest the bone.
- Allograft – bone from cadavers – DFDBA/FDBA. This was popular in the 70s/80s.
- Alloplasts – such as calcium phosphate (difficult processing as hardens quickly). Popular in the 80s/90s.
- Xenografts – bovine, porcine – now commonly used.
Hard & Soft Tissue
- Very common, especially after tooth loss.
- Aetiology of ridge defects – aetiology – trauma, traumatic extractions, periodontal disease, endodontic lesions, cystic lesions, implant failure.
- Bone healing and soft tissue contour changes following single tooth extractions (Schropp et al 2003). The majority of the changes in hard and soft tissue occur in the first 12 months of healing. Ridge preservation techniques can minimise these changes.
- Classification of ridge defects – Seibert 1983:
Class I – Horizontal deficiency, Class II – Vertical deficiency, Class III – Vertical and horizontal deficiency (combination) - Treatment – surgery is aiming for a convex ridge. Casts are useful to analyse ridge width, space and inter-arch relationship. The most common cause of failure is poor manipulation of the soft tissues.



