February 25, 2016
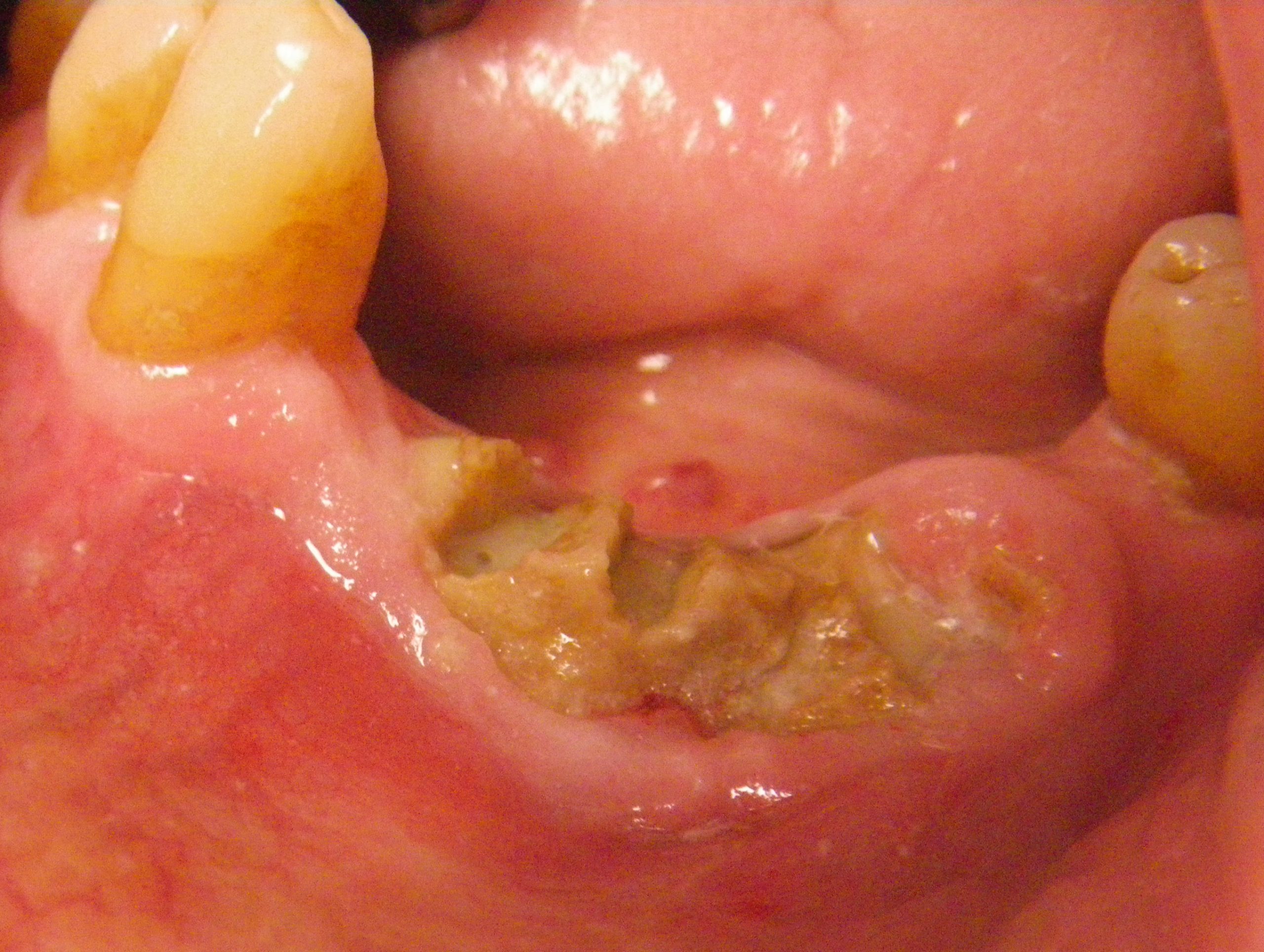
Introduction:
- Types of necrosis: MRONJ = medication related osteonecrosis of the jaw. This may be due to bisphosphonates (BRONJ), RANK-L inhibitors and anti-angiogenic drugs. ORN = Osteoradionecrosis. MRONJ and ORN have distinct differences yet many similarities.
BRONJ:
- Bisphosphonates inhibit the resorption of bone by encouraging osteoclasts to undergo apoptosis thereby slowing bone loss. Patients who may be on bisphosphonates: hypercalcaemia, tumours within the bone (multiple myeloma), cancers that spread to the bone (Breast, Prostate, Lung commonly), osteoporosis, long-term steroid use, Pagets, fibrous dysplasia.
- BRONJ (now known as MRONJ) is diagnosed as exposed or probable bone via a fistula present for 8 weeks following bisphosphonate use with no head and neck radiotherapy and the absence of metastatic disease.
- Incidence – 10/million/year = 620 new cases/year. For Oral BisPs in post menopausal women 1 in 1262-4419 (FGDP). Oral BRONJ risk – Marx showed that 3 years (156 consecutive weekly doses of Alendronic Acid) was a significant threshold marker for developing BRONJ but risk still low. This has been superseded by AAOMS who state 4 years of oral bisphosphate use for risk of BRONJ.
- Staging – 0 (no clinical evidence of necrotic bone but non-specific clinical findings and symptoms), 1 (exposed bone but no symptoms), 2 (exposed and necrotic bone associated with symptoms), 3 (exposed and necrotic bone with pain, infection and extending beyond the alveolar bone/resulting in pathologic fracture, extraoral fistula, oral antral/nasal communication, or osteolysis extending to the inferior border of the mandible/sinus floor).
- Drug holiday – varying opinions on this depending on which theory of BRONJ you accept. Most places in the UK do not take recommend a drug holiday as the half-life is long and this is usually not possible for cancer patients.
- Antibiotics – no evidence for their prophylactic use. Antibiotics for the treatment of BRONJ – doxycyline for chronic infection and if acute flare up then amoxicillin and metronidazole.
- Surgical management – case reports suggest local flaps with saucerisation and primary closure or segmental resection.
- Implants – if on oral bisphosphonates then warn patients of the risk. Contraindicated for IV bisphosphonates.
RANK-L inhibitor:
- Denosumab – potential to replace/substitute bisphosphonates. Necrosis of the jaw already recognised as a complication. Shown to be equally or more effective than bisphosphonates at preventing bone loss in osteoporosis, rheumatoid arthritis and cancer treatment with metastases.
- RANK-L inhibitor vs bisphosphonates – both inhibit osteoclasts but bisphosphonates internalised and Denosumab extracellular. Bisphosphonates are recycled, have a long half-life and a strong affinity for hydroxyapatite and bone mineral (can lead to uneven uptake). Denosumab has no sustained binding to bone surfaces, better distribution, effects bone turnover quickly and is reversible with discontinuation.
- Same presentation and management as BRONJ.
Anti-Angiogenic agents:
- Osteonecrosis of the jaw reported with bisphosphonates plus anti-angiogenic drugs. Can also cause osteonecrosis without bisphosphonates through oral mucosal breakdown, impaired angiogenesis and potential for reduced bone remodelling.
- Watch out for – Bevacizumab, Sunitinib, Cabozantinib, Sorafenib, Sirolimus and Radium-223.
ORN:
- No agreed definition!
- Incidence 4.74-37.5%, mandible > maxilla, time is NOT a healer.
- Risk factors – radiation with higher risk when: tumours affecting the mandible (tongue, FOM, retromolar, alveolar ridge), tumours of the maxilla (nasopharyngeal), adjuvant chemotherapy and a dose 60Gys (threshold). Other risk factors – trauma, infection, immune deficiencies, malnutrition, oral hygiene, alcohol and smoking.
- Pathophysiology – radiation induced fibro-atrophic mechanism
- Presentation – exposed bone – symptomatic/asymptomatic, actively infected, present for a duration of time, fistula.
- Management : Prevention – avoidance of extractions, Established ORN – pentoxifylline & vitamine E, antibiotics, surgical debridement with primary non-tension closure or if large referral to OMFS for vascularised free tissue transfer.
Referral: Guy’s Hospital (Oral Surgery Dept) accept referrals to the jaw necrosis clinic for patients on oral/IV bisphosphonates/RANK-L or anti-angiogenic drugs who have established necrosis or have a risk of jaw necrosis for oral surgery related procedures.
Further reading: New cancer therapies and jaw necrosis – BDJ, V Patel



