Home/Articles
/ Periodontology /
Reena’s Notes: 15 Key Points on the Treatment of Bony Defects caused by Periodontal Disease with Dr Nik Pandya
January 15, 2017
Periodontal Disease
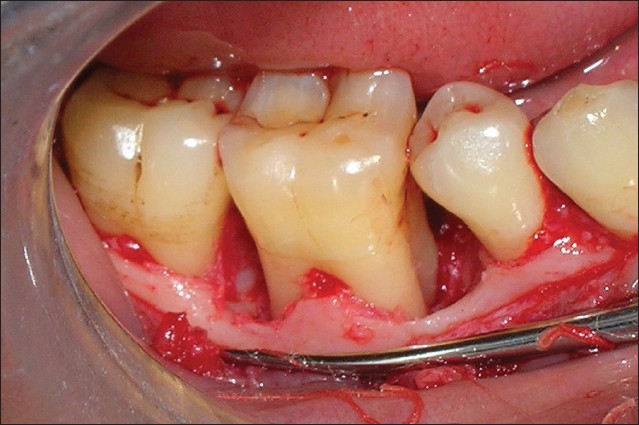
- Periodontal disease results in loss of supporting structures including alveolar bone. When the periodontal lesion results in the development of an intrabony defect, the base of the pocket is apical to the wall of the bone. Intrabony defects can be further classified as 1-, 2- or 3-walled defects. When a suprabony pocket develops, the base of the defect is coronal to the wall of the bone.
- As well as horizontal and vertical/angular bone loss, other bone destruction patterns in periodontitis include: osseous craters, reverse architecture, bulbous bony contours, ledges and furcation involvement.
- When studying radiographs and considering bone loss it is important to remember that radiographs only show mesial and distal bone levels.
- Why is it important to consider the bony anatomy when assessing and treating periodontal patients? Deep intraosseous defects are a major challenge for the clinician and are at a higher risk of disease progression (Papapanou et al 1991). Furthemore, the current approach to periodontal therapy includes regeneration of lost periodontal support wherever feasible and certain modes of treatment/materials work better with particular bony defects.
- Treatment of bone deformities caused by periodontal disease can be through non-surgical therapy or surgical therapy (resective/conventional or regenerative approach). With non-surgical therapy and conventional surgical therapy, true regeneration appears to be limited to the most apical part of the defect. Regenerative approaches to addressing bony defects may consider the use of membranes, grafts and biological agents.
- Regeneration of periodontal defects involves formation of new cementum, new attached periodontal fibres and new bone in a region previously destroyed by periodontitis. True regeneration can only be verified by removing the tooth and surrounding bone for histologic evaluation. Radiographic evidence of bone fill post surgery is not reliable because of the variation in angulation and processing of the film.
- Guided Tissue Regeneration (GTR) is one of the most frequently documented reconstructive procedures. A biocompatible membrane (resorbable or non-resorbable) is surgically implanted to isolate or protect the bony defect. If non-resorbable, the barrier is surgically removed 4-6 weeks after implantation. Connective tissue and bone regeneration might then occur within the bony lesion protected by the barrier. The biological rationale of the procedure is based on the prevention of migration of epithelial periodontal tissues into the osseous defect, allowing time for bone and other attachment tissues to heal. Example of membranes materials include: PTFE (Tefgen, BioBarrier), collagen (BioGide) and calcium sulplate (Cema, Calcigen).
- Graft materials may include: autografts (transplant from one region to another in the same individual), allografts (transplant from one individual to a genetically non-identical individual of the same species), xenografts (transplant from one species to another) or alloplasts (synthetic or chemically derived bone substitute).
- Autogenous bone is regarded by most clinicians as the “gold standard”. Examples include osseous coagulum collection from the mandible/maxilla and hip marrow graft (largely cancellous bone). However, there is minimal standardised data (mostly based on case reports) and data shows limited clinical results. However the advantages include: no risk of disease or rejection, no additional cost of material and influence of a commercial sponsor.
- Examples of allograft include: Allosource DFDB (human derived type I collagen), Pacific Coast DFDB (deminieralised human cortical – osteoinduction attributed to protein), Grafton (demineralised bone matrix, contains glycerol), Rocky Mountain (irradiated cancellous human bone). Most are effective but some have concerns over cross infection and a variable material source may lead to lack of consistency. All readily commercially available products are from the USA and have been FDA approved. Donor bone is typically screened for: HIV1&2 antibody, Hep B surface antigen, Hep B core antibody, Hep C antibody, Syphilis, Human T-lympotropic virus type I antibody.
- Examples of xenografts include: Bio-Oss (“natural” bovine derived deproteinised hydroxyapatite) and PepGen – Osteograft N-300 (similar to above Bio-Oss plus P-15 peptide
- Bioactive glass (Perioglass), hydroxyapatite (Perma, OsteoGraft D), tricalcium phosphate (Resorb, Cerasorb) and polymers (Fisiograft) are examples of alloplasts.
- Emdogain contains Enamel Matrix Protiens, or bioactive molecules, called amelogenin proteins (porcine derived in a PGA carrier). This material is works well in 3-walled intrabony defects. Other popular bioactive molecules include platelet rich plasma (PRP), plasma derived growth factor (PDGF) and bone morphogenetic proteins (BMPs).
- GTR and graft materials may be seen as the first generation regenerative materials. Biologicals such as Emdogain and PRP may be seen as second generation. Third generation therapy for periodontal regeneration may include pharmacological application of recombinant human growth factors.
- Properties of an ideal augmentation material: safe and biocompatible, osteoinductive, bioresorbable to enable complete bone regeneration, space keeping capabilities during bone formation, easy handling/technique insensitive, shortens procedure time and period to final rehabilitation, predictable and inexpensive. Current graft materials do not meet all augmentation requirements but there are exciting developments in this field. It is important to remember that the practitioner skills and experience are major factor in getting optimal results.
These notes have been adapted from a webinar organised by the BSP. To find out about similar events and to access other resources, please visit – www.bsperio.org.uk.
To learn more from Reena Wadia on Periodontal disease and more, make sure to read more from our articles and education.



