Home/Articles
/ General Dental /
Reena’s Notes: 10 Key Points on the Modern Management of 3rd Molars with Dr Chris Sproat: Less may be more?
May 7, 2016
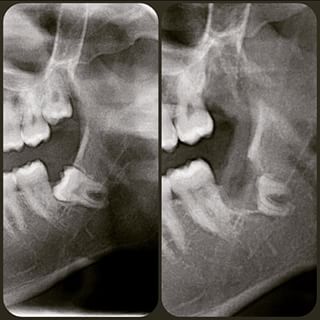
- The incidence of ID nerve damage/neurosensory deficit after lower third molar surgery ranges from 0-8.4% (Leung & Cheung 2010). This is a relatively small percentage but when it does occur the consequences can be profound. One of the most significant outcomes includes permanent altered sensation and pain in the orofacial region, which may lead to considerable functional and psychological disability.
- Injury is usually caused by manipulation of the ID nerve bundle or adjacent tissues. The risk is higher with: increasing age, deeper and more distoangulated third molars as well as a less experienced operator.
- Risk may be assessed radiographically and 3 important signs to look out for include: loss of cortical lines of the ID canal, banding across the root and deviation of the canal. However, radiographs only provides a 2D image, they can be subjective and the quality of radiographs is variable. Furthermore, 15% of patients may not have radiographic signs and still end up with nerve injury (Rood 1990). To improve our assessment it is important we look more critically at plain films and order additional views when indicated.
- A CBCT provides a 3D view with high spatial resolution, it improves our knowledge of the operative field and has high specificity when there is no risk. It can also lead to improved management of patient expectation. Most of the time, scans push us to take a more conservative approach. However, there is no evidence yet that it reduces the injury rate.
- We should make every effort to improve our techniques to reduce the incidence of iatrogenic ID nerve damage. Technique is one variable that is in our control. Various methods of risk reduction have been suggested including: avoiding surgery (NICE guidelines), orthodontic extrusion, staged removal, pericoronal ostectomy and coronectomy.
Coronectomy
- Should definitely be considered in high-risk cases. It’s technique sensitive and needs training (it’s not just half an extraction!). There is lots of evidence on this approach and the injury rate/risk of paraesthesia/ dysesthesia versus extraction is always lower (Long et al 2012). According to the evidence, for every 17 patients who have a coronectomy, you will protect 1 from injury. The procedural failure rate is low and when comparing the risk of infection against extraction there is no difference. Current follow up is 3 years (Leung and Cheung 2012) so long-term evidence is not yet available.
- The technique involves minimal bone removal, no routine lingual retraction, careful reduction of the root by 3-4 mm, removal of the pulpal tissue, meticulous check to ensure no retained enamel, sectioning with minimal finger pressure, primary closure and no routine antibiotics.
- Contraindications for coronectomy – existing caries with pulpal involvement, significant immune compromise, jaw radiation, pre-orthognathic surgery, apical pathology and significant risk from the coronectomy cut.
- No associated pathology associated with retained roots so far. Roots do migrate, leaving a ‘migration lucency zone’ made of immature bone. Don’t get caught out and think this is a periapical area. Migration is always away from the ID canal and most of it occurs in the first 6 months. Other changes that may occur include root hypercementosis or resorption.
- If there are complications a decision may need to be made on whether to monitor, perform a re-coronectomy or retrieve the root. A CBCT may be useful at this point. The final decision will be dependent on the patient’s symptoms and preferences.



